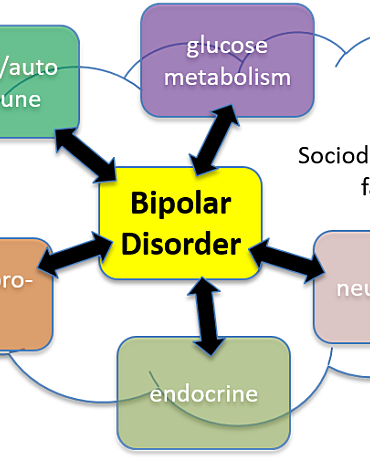
In the depressive phase, individuals with bipolar disorder may have persistent feelings of sadness, anxiety, guilt, isolation, hopelessness, disturbances in sleep and appetite, fatigue and loss of interest in activities they usually enjoy.
In the manic phase, an individual may have an increase in energy, grandiose or delusional ideas, racing thoughts, and a decreased need for sleep.
In addition to mood disturbance, an individual can also suffer from psychotic episodes, suffering a loss of contact with reality and may report hallucinations, delusions and exhibit personality changes. Some people will also experience thoughts of death and suicidal behaviors.
Individuals suffering from bipolar disorder can exhibit different patterns of mood disturbance, with individual phases lasting days or months or being mainly manic or depressive in presentation, resulting in a clinical diagnosis of any of the six different forms of bipolar disorder.
Our research approaches
Our research focuses on identifying the biological causes of and contributors to bipolar disorder. We have been recruiting individuals with bipolar disorder and their family members for more than 15 years to map the genetic contributors, and study the transmission of DNA through individual family members.
The aim of this work is to identify regions of the genome which are commonly inherited in individuals who have been diagnosed with bipolar disorder, as compared to family members or unrelated individuals who do not suffer from mood disturbance.
Our research discoveries
We have identified a number of areas of the human genome which may contain susceptibility genes for bipolar disorder.
Genetic approaches combining genome sequencing and transmission in extended families are promising strategies for gene discovery. In a study of 117 individuals from 15 extended families with multiple affected relatives, we found rare predicted pathogenic variants shared amongst affected relatives were overrepresented in genes that are involved in synaptic transmission of neurotransmitters. We found that variants that arise spontaneously in the genome (de novo) may also contribute to mutational load in people with bipolar disorder from multiplex families, as previously observed for multiplex autism families.
Our research into the predictors of illness onset relies on a cohort of young people (aged 12-30) who have a close relative with a diagnosis of Bipolar Disorder, and a comparison group of young relatives of unaffected people. We have followed these individuals with yearly clinical assessments, brain neuroimaging and biospecimens over multiple years, and are using these data to identify and understand the order of symptom presentation, and the biological features that can help predict who in a high risk group are more likely to become ill themselves in the future.
One gene we identified is involved in early brain development which, when defective, may result in inappropriate neuronal connections affecting brain plasticity. This gene defect may render the brain more vulnerable to secondary genetic and environmental insults into adulthood.
Our patient samples have also contributed to large international collaborative studies aimed at identifying common genetic susceptibility factors for bipolar disorder, specific symptoms, and treatment response, via the Psychiatric Genomics Consortium and the Consortium of Lithium Genomics, as well as differences in brain structure or function via the ENIGMA consortium.
These research efforts continue to rapidly uncover more genes and genetic variants, improving our understanding of the biological pathways involved.